- Research models
Local and systemic therapy
- We want to know why current therapies, either local or systemic, do not work well against brain metastasis.
A clinically-compatible drug-screening platform based on organotypic cultures identifies vulnerabilities to prevent and treat brain metastasis.
Zhu L, et al. EMBO Molecular Medicine. (2022).
STAT3 labels a subpopulation of reactive astrocytes required for brain metastasis.
Priego N et al. Nature Medicine. (2018).
Stratification of radiosensitive brain metastases based on an actionable S100A9/RAGE resistance mechanism.
Monteiro C, Miarka L, et al. Nature Medicine (2022).
Protocol to generate murine organotypic brain cultures for drug screening and evaluation of anti-metastatic efficacy
Lucía Zhu, Lauritz Miarka, Patricia Baena, María Perea-García, Manuel Valiente. STAR Protocols (2023)
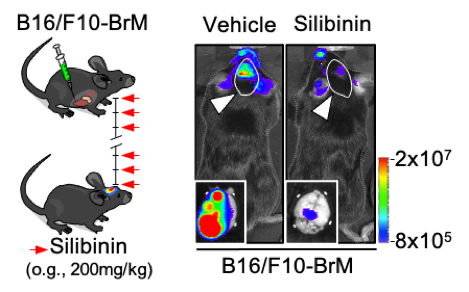
Local and systemic therapeutic approaches face different limitations to show full potential in the brain:
It is obvious that many clinical limitations require experimental models to be able to provide underlying molecular mechanisms and thus new strategies.
We have followed very different approaches to study various aspects of therapeutic failure. Traditional experimental models have been improved with neurosurgeries or irradiation protocols mimicking the clinical situation. Additionally, systemic therapies have been also incorporated. By doing so, we interrogate both cancer cells and the surrounding microenvironment at the molecular level to design approaches that make these therapies work better.
Over the years we have been able to study the process of relapse post-surgery, identify biomarkers of response to radiotherapy and radiosensitizers, identify available drugs that had never been used against brain metastasis but that turned out to be effective, improve the delivery of targeted drugs to the brain and expand immunotherapy strategies to work better in the brain.
By focusing on brain metastasis, we aim to demonstrate that either available or new strategies delivered locally or systemically could be used effectively to challenge this unmet clinical need. Our approach is focused on the brain but we are aware that most patients have metastatic disease spread to other organs and that the metastatic brain could also have important implications out of the central nervous system.